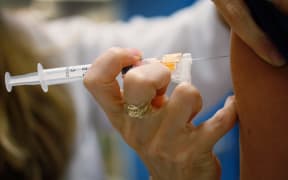
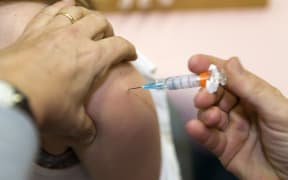
The Health Ministry is considering moving to a two-dose vaccine to protect girls against cervical cancer and genital warts.
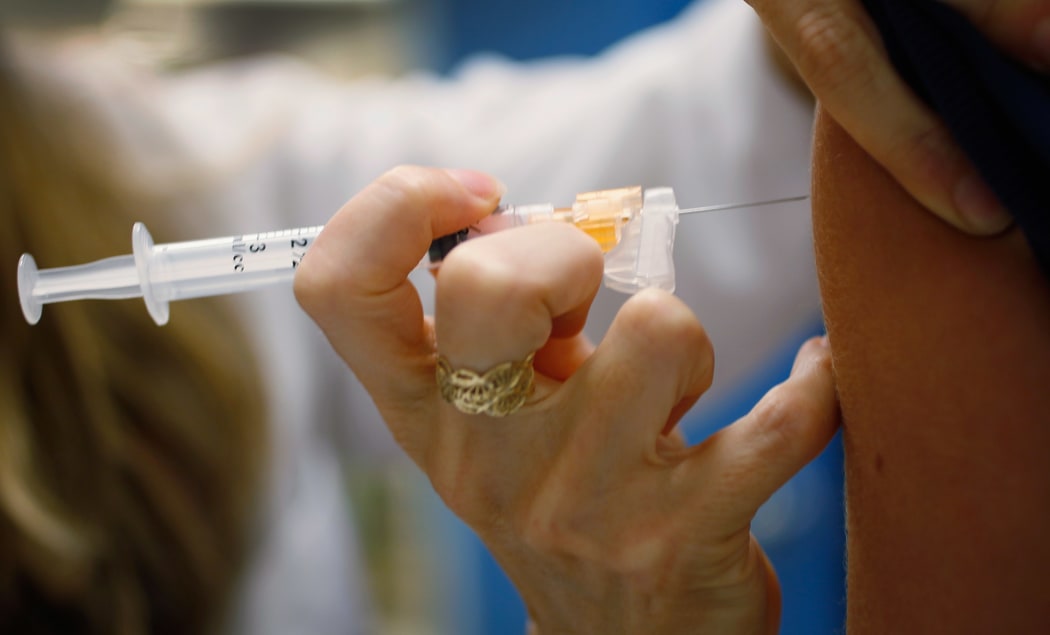
A 13-year-old girl is given an HPV vaccination in Miami, Florida. Photo: AFP
The current Gardasil vaccine against the human papillomavirus, or HPV, is used in three doses, and the uptake is low.
Every year, an estimated 30,000 girls aged 12 or 13 become eligible for the immunisation and are encouraged to be vaccinated free against HPV under a nationwide programme which costs more than $8 million a year.
The vaccine protects against the cancer-causing virus, but just 60 percent of girls receive all three jabs and are successfully immunised.
Ministry chief advisor Bryn Jones said New Zealand lagged behind other countries, and should aim to lift coverage to 75 percent by late 2017.
The Ministry was also in discussions regarding whether the vaccine could be delivered as a two-dose regimen, as it is in the United Kingdom, he said.
"It is more about technical issues about implementing a change in the programme. Also we'd like to see that the effectiveness is not decreased at all and the UK programme provides us with a good way of keeping an eye on that as well."
Auckland University Immunisation Advisory Centre head Nikki Turner was also in favour of the change.
"It's much easier for the girls to only have to have two injections. It's much easier for public health nurses to only have to deliver two injections, particularly within a short school year.
"It's then easier to recall girls who are lost or who have been lost to follow up."
The money saved could then fund the HPV vaccine for boys, she added.
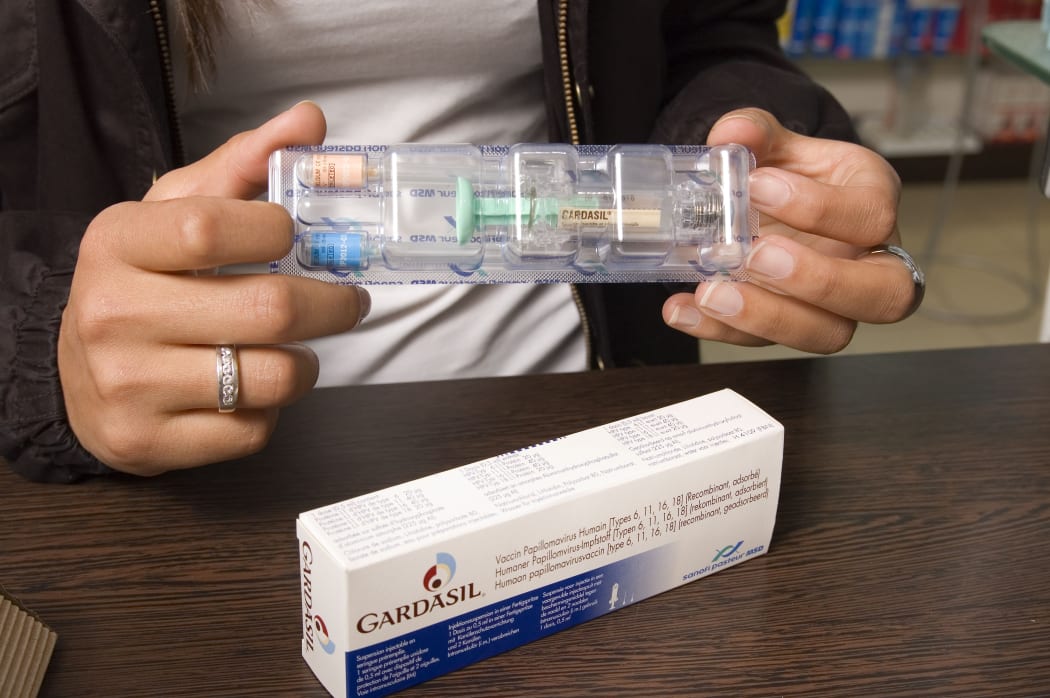
Gardasil is funded for Year 8 girls in New Zealand but doctors want that to be extended to boys and young men. Photo: BELMONTE / BSIP
Dr Jones said family doctors were being encouraged to do more to vaccinate girls who miss the jab at school.
"What we're trying to do is ensure that general practices put in place recall systems so that if they're notified that a girl has decided that they would prefer to have their vaccinations through general practice, that that is followed up by the general practice proactively."
Medical Association General Practice Council chair Kate Baddock said there were gaps in the vaccination system for girls.
"If someone doesn't turn up for their third Gardasil [injection] we don't know straight away.
"In fact, the only way we know is if we see the girl for something else and we have it noted that an immunisation is overdue.
"If we were notified immediately that somebody hadn't had their vaccination, or had declined their vaccination, then we could put some resource towards trying to follow that through, but we don't have that information in a timely way."
Immunisation Advisory Centre research director Helen Petousis-Harris said girls and their parents had different reasons for opting out of the jab at school.
One of the reasons was a mistaken belief that the vaccine might not be long-lasting and therefore it would be wiser to do it later.
But Dr Petousis-Harris said that was wrong and the vaccine might provide permanent protection, but it was essential that it was given early, before any sexual activity began.
"It's vital that the vaccine is given before infection [with HPV] occurs, and infection is most likely to occur any time from the first sexual intercourse."
Dr Petousis-Harris said health survey data showed that a fifth of girls have had sexual intercourse by the age of 13.
Cancer Society medical director Chris Jackson said while parents might feel that girls who are not yet sexually active do not need the vaccine, immunising them was a top priority.
"In actual fact, that's exactly the group that would benefit most from the vaccine prior to first sexual activity.
"It's very clear that vaccination has a major impact on the death rates from cervical cancer, it can be prevented from good vaccination coverage rates".
Otago University Associate Professor Nick Wilson said shifting to a two-dose vaccine would improve coverage among girls, and that should be done as soon as possible.
He said combining delivery of the HPV vaccine with funded injections for Tetanus Diptheria and Pertussis (TDP) at age 11 would also make sense.
Dr Wilson said if parents opted not to take up that opportunity at age 11, they should have to fund the vaccine themselves if they want it for their daughter later.
"We shouldn't be giving them lots of opportunities which mean that parents just put it off."