For one 28-year-old New Zealander, infertility was a club she never dreamed she would join - least of all at her age. She talks about her own journey, and those of others who face never having children.
Photo: 123RF
Scrolling through Facebook, a photo catches my eye. It's a set of adult Nike trainers and ballet flats, with a pair of baby booties, captioned Coming in November 2016! I don't know the person who posted the photo, and it's only because a friend liked it than I'm seeing it at all. A Facebook algorithm has determined it may interest me.
What the Facebook algorithm doesn't know is that for many people, seeing those photos - and the congratulatory comments that follow - are akin to a stab in the heart.
These people are members of a club that no-one wants to join. It's an exclusive club, this one. Either you're in it or you're not. All you have to do to join is have trouble conceiving naturally. In other words, be infertile.
The clinical definition of infertility is set by the World Health Organisation, and it leaves little room for interpretation: "Infertility is a disease of the reproductive system, defined by the failure to achieve a clinical pregnancy after 12 months of regular, unprotected sexual intercourse."
Disease. System. Failure. Clinical. It's pretty black and white.
Approximately one in five New Zealanders will experience infertility. Take a look around your office or your favourite cafe; chances are, someone in the room will be silently struggling.
'What the hell is wrong with me?'
Auckland photographer Lauren Indrisie is a member of the club. The 33-year-old and her husband Joseph started trying for a baby in April 2013. Months went by without a positive result.
"I was 30 by the time we started trying, so I knew it could take a while," says Lauren. "But every month it doesn't work you get a little bit sad. Some people would say to me, 'It might take years', but that doesn't discount the fact that six months is a long time of getting excited and hoping it'll work. Then when it doesn't work you start questioning if there's something wrong."

A couple aged 29 have a 23 percent chance of conceiving naturally each month. Photo: AFP
Working as a wedding and portrait photographer meant Lauren had to put on a brave face for her clients, even though it was the last thing she felt like doing.
"Every weekend I'm photographing happy people who are getting married and talking about having kids. I didn't want my issues to affect my personality or my happiness for other people. Every month it didn't work, I would go and buy myself a nice bottle of wine and celebrate the fact that I could still drink wine.
"The toughest thing was between Joseph and I," she continues. "Guys want to fix things. They're like 'Is there something wrong with you? Is there something wrong with me? Are you too stressed at work? Maybe you need to relax more?'"
The only inkling Lauren had that something wasn't right was a sore belly-button that wouldn't go away. Numerous visits to the GP resulted in prescriptions for antibiotics and creams, to no avail. Eventually she underwent surgery under the private health system where the belly button pain was discovered to be an umbilical hernia with endometriosis inside.
"I knew there was something wrong but I just didn't know what it was," she says. "I had all the ovulation testing kits and the fertility apps on my phone. We were trying on all the right days and nothing was working."
Further surgery followed and resulted in the removal of the endometriosis from Lauren's bowel and bladder. A month after the surgery, she became pregnant with her son Samuel.
"I'm lucky that mine was such a simple fix," Lauren says. "If I hadn't given myself that umbilical hernia, which I'm pretty sure I gave to myself during a pump class, I'd probably still be sitting here wondering what the hell was wrong with me."
'Is this karma?'
41-year-old Mandy* is also childless, but not by choice. The Auckland-based account manager met her current partner Andrew at 32. At 37, after getting married and buying a house, they turned their attention to raising a family, not realising what a long journey it would be.
"We tried for about a year-and-a-half, almost two years all up," Mandy says. "I had a really stressful job at the time and was working exceptionally long hours. I was so naive. I didn't even think about things like a fertility test."
Mandy had had stomach pains, bloating and painful periods for some time, which she and her doctor assumed was gut-related. When eliminating gluten didn't relieve the symptoms, her doctor referred her for an internal ultrasound.
"I went and had the scan and they said, 'Oh, you've got a few cysts on your ovaries'. I didn't think much of it at the time. I got called back in to have some cancer tests, but they were 99 percent sure it wasn't cancer."
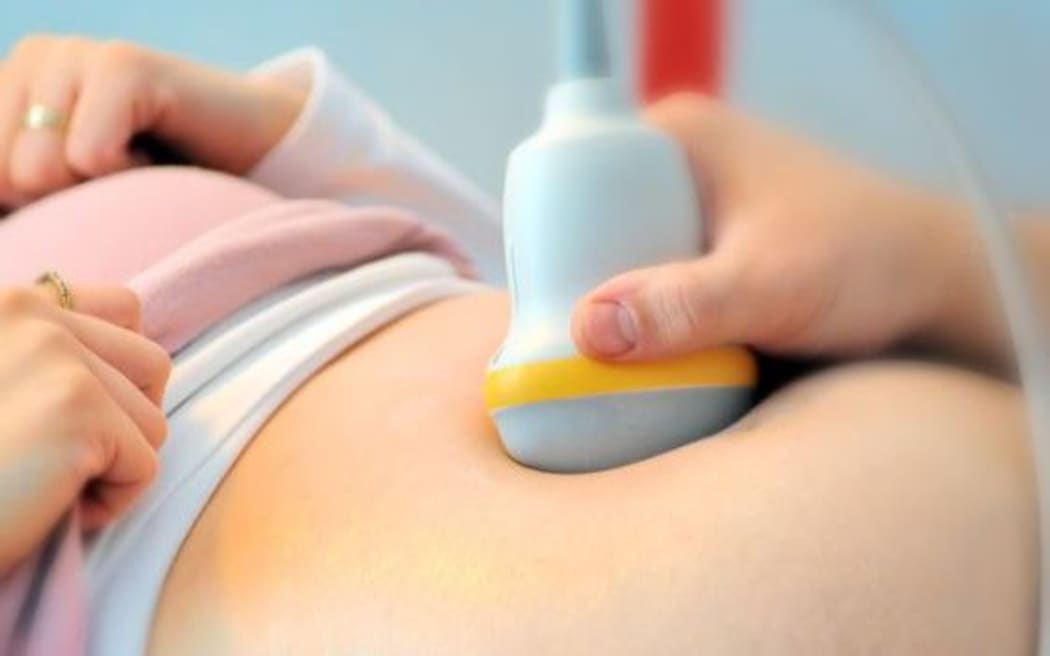
Mandy urges women to get checked out if they're having problems with their periods. Photo: 123rf
An operation was planned to remove the cysts, but before the surgery date, Mandy's ovaries twisted. Both ovaries had to be removed in an emergency surgery, and tests afterwards revealed cancerous tumours inside.
"It was pretty rough, to be honest," she says. "I went from having cysts to possibly having cancer to definitely having cancer to not being able to have children of my own to going into menopause."
Most people would assume that Mandy and Andrew would turn to adoption, but due to both her age and Mandy's cancer experience, that's not possible.
"I talked with the fertility specialist about adoption, and she just said to me, 'Mandy there is no way anyone will give you a baby because you're over 40 and you've had cancer'. That was pretty harsh for someone to say so baldly.
"I got really depressed around then, and I had some grieving to work through. You do stupid things like think 'Is this karma from being mean to someone, or from stealing a pen from work?'. All those awful bad things that you never tell anyone. I spent a lot of time thinking about what I might have done to cause my cancer."
"It's difficult when people ask you about having kids," she adds. "It took me a long time to think of what to say. I used to say, 'I've had cancer,' and explain the whole thing, but now I just say 'No'. For me it's about shutting down the conversation. No one needs to know why I can't have children."
Mandy and Andrew are currently working with a fertility clinic to produce an embryo conceived with a donor egg and Andrew's sperm. If the embryo is created successfully, Mandy will carry the pregnancy.
"I think it really helps for women to think about their periods a lot more," she says. "If you've got stomach pains and really bad periods, don't just think it's normal. Go and get checked out."
Searching for sperm
Lara* and her husband Chris* are also unable to have children of their own, although unlike Lauren, there is no apparent medical reason for why Lara can't conceive. Chris, however, has Klinefelter's Syndrome, a genetic condition that has rendered him infertile.
Men with Klinefelter's Syndrome have an extra chromosome that results in a testosterone deficiency, weak muscles, and above-average height. Diagnosed with the condition as a child, the impact of the syndrome on his fertility was nonetheless never discussed with him. The couple started trying for a baby when Lara was 36. A year went by with no success before Lara approached her GP.
"I got some tests done and they all came back as relatively normal," explains the 39-year-old sales manager. "They told me to keep trying, to avoid alcohol and lose weight and take vitamins."

Photo: 123RF
Another 18 months of trying would go by before Lara convinced her GP that something wasn't right and maybe Chris should be tested as well.
"Chris got tested and that was when they found out the extent of his Klinefelter's Syndrome," says Lara. "He had pretty much a zero sperm count. Finding out about Chris was the biggest shock.... We haven't had a lot of time to sit and dwell on it. We've had to think quickly about what we do and how we do it."
A sperm retrieval procedure was performed, but wasn't successful. The couple then decided to find a sperm donor.
"It's very difficult to find a sperm donor in New Zealand," says Lara. "It's not like you think it's going to be: you don't go in and flip through a book of male models. It's like online dating; you go out there and put up a profile and see what happens.
"We got a lot of responses very quickly, but a lot of them were dodgy people who only wanted to do things naturally and were happy to 'come over anytime and help out'. We didn't want that - we wanted everything to be done through a clinic and be above board.
"We went through lots of time wasters and then came across one person who sounded like a great guy. He had a very similar upbringing to Chris and I, and he'd helped another couple already. His height, hair colour and eye colour were a pretty good match for Chris, so it just seemed like a good fit."
The sperm donor was happy to proceed, and Lara and Chris will be starting IVF with Lara's eggs and the donor sperm later this year.
More awareness needed
Research quoted by fertility support charity Fertility NZ indicates that a couple aged 29 have a 23 percent chance of conceiving naturally each month, or a 48 percent chance of conceiving with IVF. As a couple gets older, those percentages drop.
Public funding for IVF is available for couples who meet certain criteria. Women aged under 40, who are a New Zealand resident and have experienced at least 12 months of infertility are eligible for a publicly funded specialist appointment. During the appointment a history is taken and various tests performed. Based on the information gathered during the appointment, a score is created which is then measured against the Clinical Priority Assessment Criteria (CPAC).
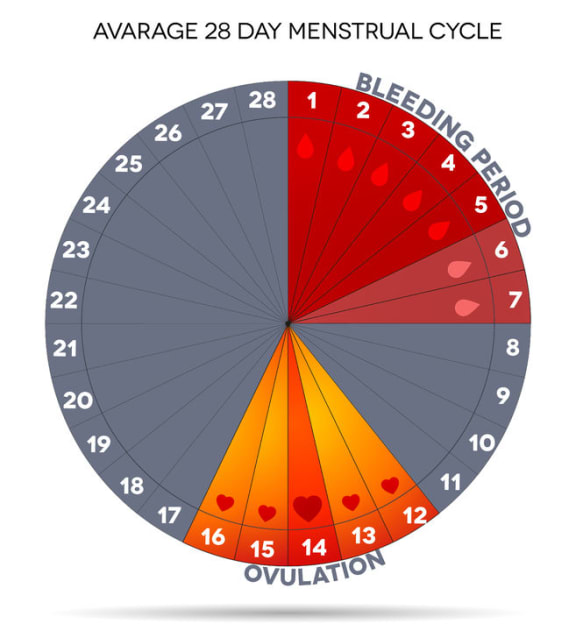
Average 28 day menstrual cycle. Photo: 123RF
To be eligible for public funding, a couple must have a score over 65. Even with public funding in place, it's not unusual to have to wait up to 18 months for treatment to begin. Starting early is the key.
"We feel quite strongly that there needs to be more awareness of fertility in young people," says Nicola Butossi of Fertility NZ. "There's lots of awareness around contraception, but there's not really any education on understanding your fertility and how it might affect you in the future."
It's a sentiment echoed by Dr Debbie Blake, scientific director of Auckland fertility clinic Repromed. "Subfertility is so often due to a combination of male and female factors," says Dr Blake. "For women there are so many signals that our bodies are sending us that we could really benefit from learning to read. Many women have painful periods that should get investigated early and even men can now easily pick up a home sperm test kit to get a rough idea of their sperm quality.
"At the end of the day, knowledge is power. The sooner you can recognise there's a problem, the greater the chance of success if treatment is recommended."
Infertility is an incredibly difficult thing to keep inside, says Lara. "You get people asking questions like 'Why aren't you drinking?' 'Why aren't you coming out?' 'Why do you have to get up at 6am on a Sunday morning to get blood tests done?' and all the s*** that goes along with it.
"I don't want people to tell me it's going to be okay," she says. "I want people to go 'Hey, we wish you all the best. Go you!' I can take that, but don't pat me on the back and tell me that everything is going to be alright."
*Tania Seward is a freelance writer who gave up a career in commerce to spend her days transforming caffeinated beverages into coherent sentences. When she's not writing she's likely to be found knitting in a public place.