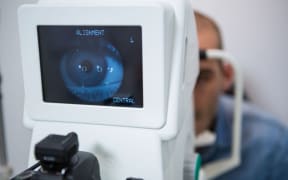
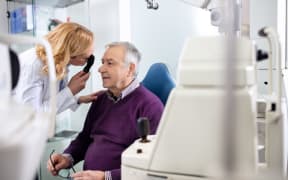
Eye specialists are frustrated about what they say is a lack of government action over a common eye disorder that can lead to blindness.
They're demanding government funding of up to $3 million a year to raise awareness about age-related macular degeneration.
Wellington businesswoman and mother Jo Gordon came close to losing her vision 10 years ago.
It began as she was looking out the window at the view. "All of a sudden the horizon on the sea became crooked, it just didn't look right, and I also got this sort of black blotch in the middle of my eye as well and it got worse overnight."
She saw an eye specialist, and was diagnosed with macular degeneration.
That is where abnormal blood vessels in the retina leak, bleed and form a scar, causing vision loss, which can worsen quickly.
The Wellington woman was worried, to say the least. "I was only 47, running a business, needed my sight of course, I had teenagers."
She was given what's now the standard treatment - an injection in the affected eye - to halt the deterioration. It is repeated whenever necessary and has saved her vision.

Dianne Sharp Photo: RNZ / Karen Brown
Dianne Sharp, the head of Macular Degeneration New Zealand, said 200,000 people in this country had some form of macular degeneration and 10 percent had lost vision as a result.
Every year 3000 more people are diagnosed or develop the more severe form - late macular degeneration.
"If those people are not picked up at an early stage that's 3000 people per year that will lose vision, and 75 percent of those people will lose vision within three years and many of them within the first few months."
Dr Sharp, an ophthalmologist, said people need to know the importance of early intervention in protecting their eyesight.
"If there is any delay, that delay may be over weeks or months, then the layers of the retina get destroyed and there's no amount of treatment that can fix that.
"Early intervention's absolutely critical."
Long waits for follow-up eye checks at several district health boards - including for those with macular degeneration - has raised the profile of the disorder recently.
But Dr Sharp wants much more done, and urged the Ministry of Health to adopt a plan developed by the former National Health Committee setting out how care should be managed in future.
She said that was vital with a growing older population and a stretched ophthalmology workforce.
British retina expert Alan Bird said treatment of the disorder had improved substantially, but there were challenges for all countries.
"It requires a lot of personnel, it may require equipment that you don't have, it means acquiring expertise that you may not have had, and this represents a problem from the ophthalmic profession but also optometrists, anybody involved in eye care."
Professor Bird said those over 60 or 65 should know about macular degeneration, particularly if it was in the family.
Wellington's Jo Gordon needs no convincing. "I can live a normal life ... it would be awful without sight, it's just you don't realise how important your sight is until it gets compromised."
The Ministry of Health said last week it was about to let a contract to continue the National Health Committee's work.