Liz McGimpsey and her husband weren’t keen on vaccinations but after nearly losing their daughter, she barely remembers why.

Photo: Illustration: Rachel Neser
The first time Liz McGimpsey flew in an airplane with her daughter, she hoped it would crash.
They were on an emergency flight to Starship Children’s Hospital in Auckland. Her critically ill baby lay in the back of the aircraft while doctors did their best to keep her tiny lungs working.
In the pit of her stomach, Liz didn’t believe her daughter would survive.
“I just wanted the plane to crash and for all of us to die right then and there,” says Liz. “It was an absolute nightmare.”
The doctors who treated the baby would later say it was one of the worst cases of whooping cough they’d seen in over a decade.
Liz’s daughter, Freda, was born 5 November, 2014, in a house-truck on a farm in Shannon. With her midwife and husband Caleb by her side, Liz’s homebirth went perfectly to plan. Freda arrived with a head of brown hair that twisted to curls at the end. She had round plump cheeks, full lips, and soft hazel eyes. She was the couple’s first child.
Liz and Caleb weren’t keen on getting Freda vaccinated. They had decided against the vitamin K shot at birth - an injection given to babies to prevent the risk of getting several rare bleeding disorders. As far as the rest of the vaccinations were concerned, they planned to delay her immunisations and then just choose a few that seemed safe.
“We weren’t hardcore anti-vaxxers but we just thought ‘why would we vaccinate?’ I didn’t want to put anything into my or her body that would cause danger to her. I wanted her to be as natural as possible,” says Liz.
“We had so many friends who weren’t vaccinating and I guess from what we had read, we had a distrust of the medical system and a distrust of the money being made off vaccines.”
Liz struggles to remember exactly why she was against vaccinations. It seems ridiculous to her now seeing as one vaccine during her pregnancy could have prevented the severity of baby Freda’s whooping cough.
The Ministry of Health recommends that children get the whooping cough vaccine at six weeks, three months, and five months of age. If they don’t, they are five times more likely to be hospitalised with whooping cough than those babies who are vaccinated on time.
The problem is that babies under six weeks old are too young to be immunised but are still highly vulnerable to catching the respiratory illness. Immunity to the disease wanes over time, even in immunised people, so all adults are a potential source of infection for babies.
Because of this, a whooping cough vaccine booster is available for all pregnant women for free. When a pregnant woman is vaccinated, her body develops antibodies which pass through the placenta and help protect the newborn from severe whooping cough for the first few months of life.
Around half the babies who catch whooping cough before the age of 12 months require hospitalisation and one or two in 100 of those hospitalised die from the disease. In around two in 1000 children, whooping cough leads to permanent brain damage, paralysis, deafness or blindness.
Liz says she wasn’t offered the free whooping cough vaccine when she was pregnant, but doubts she would’ve taken it.
“To be honest, I would have probably said 'no' anyway, which is maybe why my midwife didn’t ask.”
***
When Freda was four weeks old, she developed what her parents thought was a cold. “I distinctly remember I dipped a piece of cloth in eucalyptus and pinned it onto her,” says Liz, rolling her eyes.
Her symptoms didn’t seem too bad, so the family went ahead with a trip to a friend’s wedding. When the bride took Freda for a cuddle she felt something wasn’t quite right, commenting on how fast the baby’s heartbeat was. Later that night, Freda’s breathing started to deteriorate. She developed a seesaw-like breath, a sign that she was struggling to breath in air.
Liz and Caleb went to Wellington Hospital where Freda was immediately put on oxygen. The doctors diagnosed her with bronchiolitis - a common condition for children under two. No-one was particularly concerned and expected she would start getting better in about three days.
But over a week in hospital, with oxygen flowing through her nose, the doctors and nurses were baffled as to why Freda wasn’t improving. They decided to test her blood. Liz and Caleb grew concerned and asked the nurses how many babies die from bronchiolitis.
“We always send them home before Christmas,” Liz says the nurses told them.
But when the results came back, it was clear that wasn’t going to happen. A normal white blood cell count in a baby is between 5000 and 10,000 cells. Freda’s was close to 100,000, showing her body was fighting something serious. Doctors thought she had leukemia. The decision was made to send Freda to Starship.
“I was just a wreck. Sitting there with the electric pump, having to throw away all the milk, and thinking she was going to die,” says Liz.
Just before boarding the helicopter, Freda went tachycardic, her heart beating at a dangerously fast pace. She started having fits of coughing as she struggled to take in air. Doctors in Wellington had to sedate and intubate her, putting a tube down her throat to take over her breathing.
The hospital chaplain was called. Doctors warned that Freda might not make it through the flight. Still, no one had tested for whooping cough.
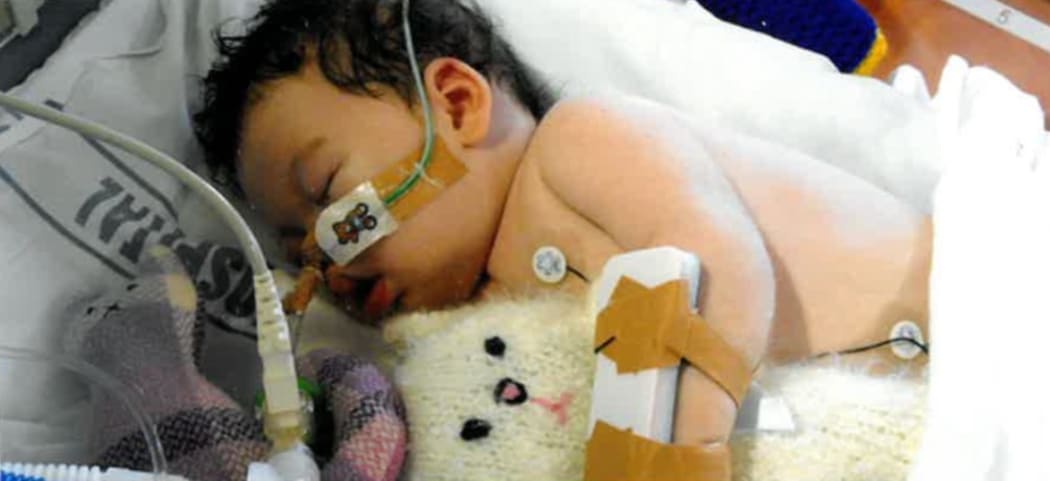
Freda McGimpsey Photo: Unknown
Outbreaks of the disease occur every three to five years in New Zealand. The most recent outbreak began in August 2011 until December 2013, with about 11,000 cases. Three young children died from the disease during this outbreak.
While there was a drop after the 2011 outbreak, there has been a gradual increase in the number of cases since mid-2016. This year, the average is about 120 cases per month.
***
“I can still smell it”, says Liz. “Those sterile corridors at Starship. You’re not there if your child isn’t very ill. It’s not a happy place to be.”
The Starship nurses took one look at Freda and knew. They’d see infant whooping cough before and Freda was showing all the signs. The tests came back positive and doctors warned Liz and Caleb that they don’t see many babies as sick as Freda survive. Her white blood count was so high that she was at risk of her own body attacking itself, resulting in organ failure.
The doctors decided to try a double blood transfusion - a risky procedure with a high chance of being rejected by Freda’s struggling body. But nevertheless, a specialist was called. She’d only ever done one other double blood transfusion on a baby so young.
“It was an absolute nightmare. I remember crying the whole time. We were told to prepare ourselves in case she didn’t make it through the night.”
The double blood transfusion took five hours. Doctors painstakingly drained her blood with a syringe, replaced her blood with a donor's, then did it all over again. Liz says that this is where many babies with whooping cough die; they get the transfusion but their bodies reject it.
Freda’s transfusions were a success but they were reminded that they weren’t out of the woods yet. “Our room was the emergency bell room. It was just constantly ringing so we could not go anywhere”.
They spent Christmas in Starship. One of the nurses from Wellington Hospital called Liz and Caleb and apologised. “She said she was carrying this guilt and couldn’t believe they didn’t think of whooping cough.”
“To be honest, maybe it was a good thing we didn’t know because then we would’ve also known that there is no treatment for whooping cough. We would have also Googled the survival rates for babies as young as Freda.”
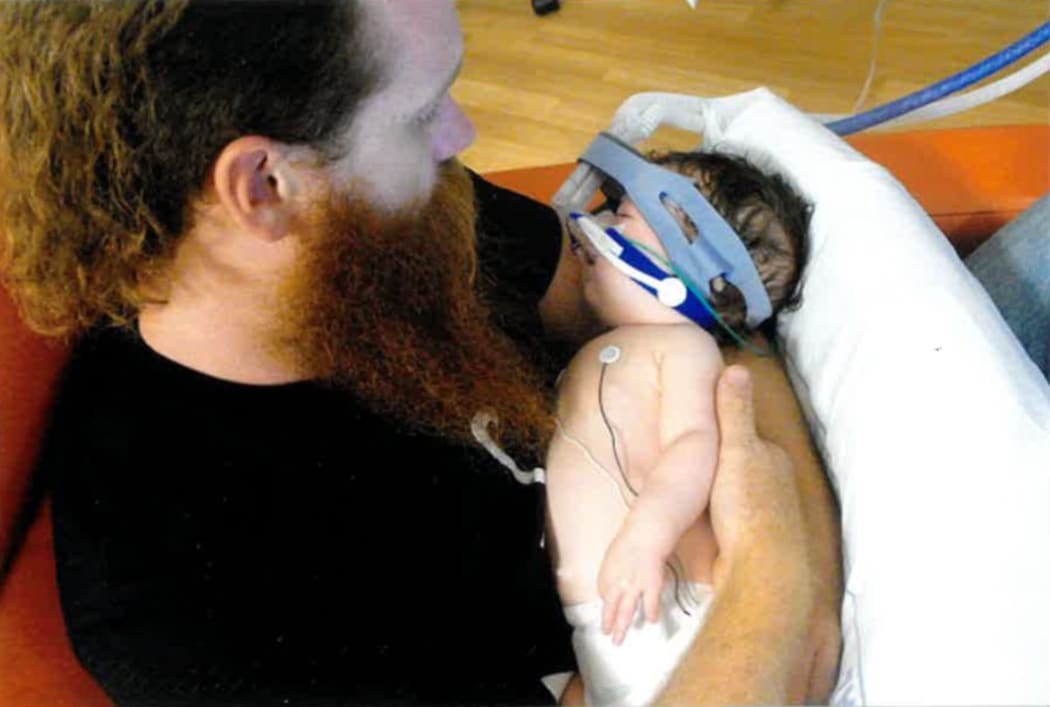
Freda and her dad Photo: Unknown
Antibiotics can be prescribed during the early stages to reduce spread of the disease, but whooping cough has to be waited out. It can last up to three months and is sometimes referred to as the "hundred day cough".
Freda was one of the worst cases of whooping cough that Starship had seen in 15 years. Miraculously, she survived.
“I remember the nurses giving us lectures about immunisations. They must see it a lot,” says Liz. While at the hospital, Liz and her entire family got the whooping cough vaccine.
Freda’s blood count started to improve but it was a long journey to recovery. She started having seizures while still under intubation and her coughing fits continued.
“Her eyes were flicking and rolling back. I just wanted her sedated so she wouldn’t be suffering through,” says Liz.
“I actually had people tell me that she should’ve just been treated with vitamin C. They have no idea that she actually couldn’t be conscious through this. Her body could not have handled it.”
On New Year's Eve, staff decided she was strong enough to be taken her off the ventilator that she had been on weeks. One of her lungs collapsed. They waited then tried again. Once she was off intubation, Freda was past the worst of it. She was carefully weaned off the drugs and eventually flown back to Wellington Hospital.
“It sounds horrible but I think that anti-vaxxers actually have to experience this to understand. I think this experience would change your mind. A vaccine compared to how many drugs were pumped into her body to keep her alive - I would prefer a vaccine any day.”
For a long time, Freda still coughed and struggled, and nurses would bag her with a manual resuscitator. Once at home, Liz and Caleb would sit her up at night during her coughing spells.
Freda came away without signs of permanent damage. She’s small for her age but Liz is grateful that she has a healthy, little girl.
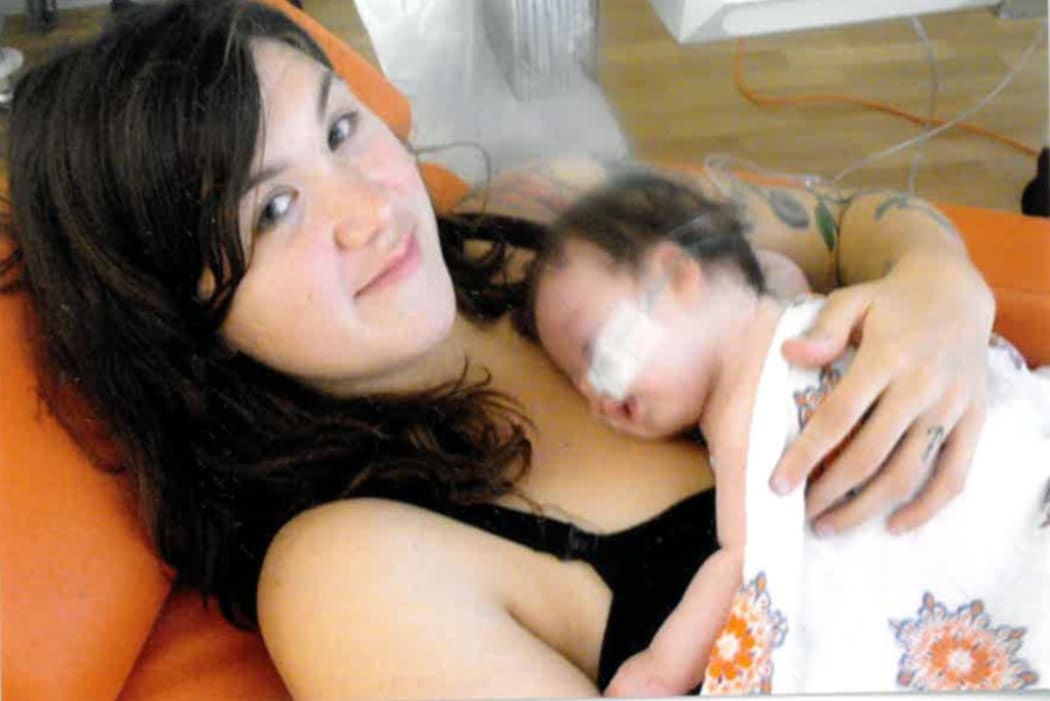
Freda and her mum Photo: Unknown
Now Liz says she’s “perplexed” as to why parents wouldn’t immunise their babies since the benefits far outweigh the risks. But she understands the amount of misinformation online can be difficult for parents to navigate.
“It’s so hard when there is so much pressure from certain people online that it really does start to bring doubt into minds of mothers. These people really do prey on vulnerable mums.”

